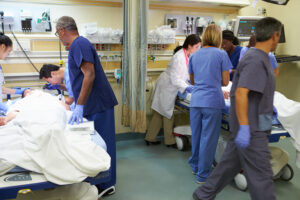
 Patients never anticipate the day when an emergency will bring them to a trauma center, so when this happens, they depend on the team of highly trained health care providers to be able to act fast and provide the best care possible. Board Certified PAs are part of that team.
Patients never anticipate the day when an emergency will bring them to a trauma center, so when this happens, they depend on the team of highly trained health care providers to be able to act fast and provide the best care possible. Board Certified PAs are part of that team.
As a Board Certified physician assistant (PA) in critical care at a trauma Intensive Care Unit (ICU) in West Philadelphia, I’ve seen the devastating impact of gun violence on patients and their families.
In response, I have partnered with my trauma center’s Injury Prevention Coordinator to become an instructor for the American College of Surgeons STOP THE BLEED® program.
STOP THE BLEED® is an educational program that teaches both medical and non-medical professionals how to properly pack wounds and use tourniquets. In the event of a gunshot wound or other penetrating injury, the knowledge and skills learned through this program can save a limb or even a life.
As part of the program, I assist in providing community outreach education and give presentations to health care organizations and area businesses. Additionally, these educational programs are incorporated into the Advanced Trauma Life Support (ATLS) certification program.
The physical damage of a gunshot wound (GSW) is severe, but the emotional toll is immeasurable.
When a patient with a GSW arrives in the hospital’s trauma bay, the trauma surgery team quickly assesses the patient for life-threatening injuries. Most patients undergo imaging to check for internal injuries, but some are too unstable and go straight to surgery.
When patients arrive in a life-threatening situation, they are at the mercy of the highly skilled and rigorously trained clinicians who are present. These clinicians work together tirelessly to save the patient’s life.
PAs, along with other health care providers, use a variety of interventions to stabilize patients with multiple traumatic injuries. Interventions may involve providing sedation, ventilating the patient, administering vasoactive medications, utilizing renal replacement therapy, using anticoagulants and organizing further surgical procedures. Depending on the location of the GSWs, patients may undergo major surgeries such as bowel resections, splenectomies, nephrectomies, liver resections, lung resections, orthopedic surgery, or other procedures.
Regardless of the inciting incident, circumstances, age, race, degree of injury, or time of day or night, these patients are relying on us to provide life-saving care. This pressure to constantly perform to the best of my ability at the top of my license is what motivates me to continue to learn and grow as a PA.
The most rewarding aspect of my career is supporting patients and their families along their road to recovery after a traumatic experience. Seeing a patient transfer or “graduate” from the ICU to the surgical floor as a result of the efforts of the entire health care team are extremely impactful.
After patients leave the hospital, my institution’s Trauma Violence Recovery Program equips social workers with specialized expertise in post-traumatic care to help them and their families plan for continued care. This may include follow-up outpatient appointments, psychological support and financial assistance through enrollment in programs that help patients and their families afford medical equipment, placement into collaborative post-acute care centers and home nursing care.
The trauma experienced by gun violence is more than just physical and extends much further than the individual patient.
PAs are an integral part of providing care to patients with life-threatening injuries. From the trauma bay to the operating room, to the ICU, PAs are there every step of the way – ensuring the highest quality of care for patients in need. PAs are there to provide the care that helps patients get through the process and can help save a life because PAs Do That!

Mary E. Herc, MSPAS, PA-C, CAQ-HM, CAQ-EM
Mary E. Herc, MSPAS, PA-C, CAQ-HM, CAQ-EM, is a Board Certified PA who works in critical care at a Level I Trauma Center in West Philadelphia, Pennsylvania. Herc also serves in the NCCPA PA Ambassador program.